Ketamine for Depression & Mood Disorders
For severe intractable Depression, Bipolar disorder, Migraines, PTSD, and CRPS or RSD [Reflex Sympathetic Dystrophy] we offer IV Ketamine Infusion Therapy in the Louisville, KY area. The results have been outstanding.
Ketamine Information
Who can benefit from ketamine therapy?
- Persons with neuropathic pain that is not well controlled with injections, nerve blocks, or prescription pain medication. Examples of this kind of pain are trigeminal neuralgia, complex regional pain syndrome (CRPS), or reflex sympathetic dystrophy (RSD), phantom limb pain, diabetic and other neuropathies, post-herpetic neuralgia, and some headaches.
- Persons with chronic back and neck pain no longer responsive to any form of treatment.
- Persons with debilitating fibromyalgia.
- Persons with other debilitating musculoskeletal and joint pain.
- Persons with resistant Depression, Bipolar disorder, PTSD, OCD, Migraine
To book a consultation, please fill out our contact form or call us at 812-913-4416!
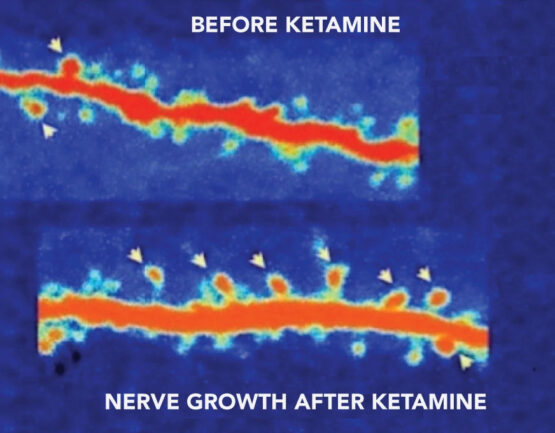
Ketamine and Depression
Patients who have been diagnosed with treatment resistant depression are candidates for ketamine infusion therapy. This includes patients with major depressive disorders, post-partum depression, bi-polar depression and severe anxiety states. When a patient has not responded to in-patient therapy, medications or other forms of treatment, Ketamine infusions should be considered as the next step.
Ketamine therapy is not for those with mild depression, situational depression, or mood swings. Severe depression is often the result of Post-Traumatic Stress. This stress does not have to be the result of “war wounds”, but can arise from neglect, abandonment, bullying, sexual abuse, or severe depravity during the developmental years. The depression is often not manifest for a decade or more following the trauma. Ketamine infusion therapy can successfully treat post-traumatic stress and subsequent depression.
Patients with recurrent thoughts of suicide, who need immediate mood stabilization, will most often benefit from Ketamine infusion therapy.
If you are visiting this website you are most likely dealing with a major depressive disorder (MDD) that has not responded to other medications. Many of you will have had trials of all the available antidepressants. Some of you have had ECT and /or TMS with no significant improvement in your condition. Chances are that you can no longer function at home, work or school, and find even small tasks, like showering, insurmountable.
Periods of depression are common mood disorders that most people face from time to time. They follow life events and disappointments that impact us deeply. These kinds of depression are generally short lived and respond to psychotherapy, conventional drug therapy or simply tincture of time. They are not crippling. But, lifelong MDDs are something different, and are more likely associated with suicidal thoughts and attempts.
Nearly all of the patients with MDD that I treat are survivors of childhood trauma. They are actually suffering from post-traumatic stress disorder (PTSD). Childhood trauma can arise from a variety of causes; abject poverty, physical, mental or sexual abuse, neglect, parental divorce, disabilities, and bullying, to name some. All of the above result in stress, anxiety, pain and feelings of low self-worth. It is these feelings that morph into MDD, beginning as early as the late teens and continue thereafter. The cause is a change in brain chemistry brought on by childhood stress, with subsequent changes in brain anatomy that are difficult to repair.
Brain Derived Neurotropic Factor (BDNF) is an important brain chemical. It is responsible for the maturation and maintenance of the neuronal dendrites and synapses that are necessary for normal brain connectivity. That is, in order to have a normal mood, the neurons in various parts of your brain need to be able to connect to each other via their dendrites and their synaptic contact. Childhood stress and anxiety inhibit the production of BDNF, leading to visible changes in neuro-anatomy and subsequent serious mood disorders such as MDD, PTSD, obsessive compulsive disorder (OCD), and anxiety.
Over the past five decades, antidepressant research and medications have revolved around the regulation of three neurotransmitters; serotonin, dopamine and norepinephrine. Together, they represent about 15% of the brain’s neurotransmitters. Much more prevalent is the neurotransmitter glutamate, which has only recently begun to receive attention as instrumental in treating mood disorders. It is via the glutamate system and two important receptors, NMDA and AMPA receptors, that ketamine works to relieve depression. It does so by turning back on BDNF production. The BDNF then leads to repair of the damaged neurons with regrowth of the important dendrites and synapses needed to achieve a normal mood. Animal models show us that the repair can begin in a matter of hours after the administration of ketamine. This process of brain repair is called neuroplasticity, and ketamine facilitated neuroplasticity offers great hope for patients with MDD who have not responded to other treatments.
Read a recent blog post about this:
Read this recent blog post about why ketamine treatment may be right for you.
IV Ketamine Infusion for Depression Patient
Our patient, Kevin, talks about his long time struggle with depression and how IV Ketamine infusion treatment changed his life.
If you or someone you know is suffering from this level of pain and or depression, contact us at 812-913-4416; 812-282-1575 today for help.
Are infusions done as outpatient?
Yes. All infusions are administered in our private office.
How do I know if Ketamine Infusion Therapy will help my pain?
While current research on the treatment of some cases of chronic pain have been promising, there is no guarantee that Ketamine Infusions will help your pain. We carefully screen each candidate prior to treatment to ensure we have the highest probability of success.
How will you determine how many Ketamine Infusions I will need?
By experience with your type of pain, and observing your response to the first six infusions. You will receive a minimum of six and a maximum of ten infusions depending on your response.
How frequently are infusions scheduled?
The best results are achieved when infusions are administered on successive days.
Will someone need to come with me?
You may arrive alone and undergo the infusion without a friend or relative present. Our staff will be watching you closely. However, all patients must be accompanied by a responsible adult at time of discharge.
What about eating and drinking on the day of my procedure?
Patients in the morning session must have no food or liquids after midnight the night before. A sip of water with medications is OK. Afternoon patients may have clear liquids until 8:00 am, then nothing other than medication with a sip of water.
I heard that Ketamine can cause hallucinations.
If given alone, sometimes Ketamine can cause hallucinations. To limit the occurrence of this side effect we sometimes administer midazolam, a benzodiazepine that is very effective. Only rarely will a patient have to stop treatment because of any of Ketamine’s side effects.
How will I feel after the Ketamine Infusion?
Your thinking may be a bit cloudy and your walk unsteady for an hour or two after treatment. There will be a few more hours of tiredness. But, hopefully there will be a noticeable improvement in the pre-treatment level of your pain as well..
What is the goal of Ketamine Infusion therapy?
What we want to achieve is a significant reduction in your level of depression/anxiety and a significant improvement in the level of your pain. With a decrease in your depression, anxiety or pain you can expect to increase your activity level and improve your overall quality of life.
How long will my depression and pain relief last?
Following a series of infusions we want to see a prolonged period of significant depression and pain relief measured in weeks to months. Most patients will need to return from time to time for a booster infusion to maintain that level of relief.
The Science of Ketamine
Four out 5 ketamine patients experience moderate to excellent pain relief. Often months of lasting relief. Immediate results in patients with refractory depression.
The NMDA Receptor
The dorsal horn of the spinal cord is important for the transmission and modulation of pain signals arising in the periphery. An important receptor in the dorsal horn is the NMDA receptor. Peripheral pain causes the release of glutamate which binds to this receptor. This results in an opening of the NMDA receptor channel allowing the influx of ions which leads to a cascade of neurochemical events ending with pain perception by the brain. With prolonged stimulation of these receptors, a central sensitization occurs. Ketamine blocks the NMDA receptor and stops the transmission of peripheral pain signals to the brain. With prolonged blockage during Ketamine Infusion Therapy, the brain “reboots” and stops interpreting peripheral stimulation as pain.
Ketamine
Ketamine is not a new drug. It has been used for five decades in human and veterinarian medicine. Most commonly it has been used as a general anesthetic agent. In anesthetic doses it results in a complete loss of consciousness while preserving certain protective reflexes. That has made it attractive to anesthesiologists in selective patients. While it does stimulate opiate receptors, much like morphine, its action in sub-anesthetic doses as an NMDA receptor antagonist is much more important in the treatment of chronic pain. By blocking the receptor and closing the channel to ion transport, pain signal transmission is interrupted giving central pain centers a chance to “reboot”. One or a series of low dose ketamine infusions in awake patients can dramatically alter or even eliminate their chronic pain. Ketamine infusions have been most often used when other treatment modalities have been less effective. Certain types of pain considered to be “neuropathic” in origin have been most studied and are considered to be most responsive to ketamine therapy. However, other types of chronic pain such as chronic temporal mandibular joint (TMJ) pain, some headaches, and musculoskeletal pain may also benefit from ketamine infusions. The list of chronic pain syndromes that benefit from ketamine therapy continues to grow.
Ketamine Side Effects
Ketamine infusions are generally well tolerated, and few patients need to terminate treatment because of side effects. Still, ketamine is a derivative of phencyclidine (PCP) a known psychedelic and if not combined with sedation can cause hallucinations in many patients. You will be given a benzodiazepine to control this dysphoria. Other possible side effects include nausea and rarely a headache. These side effects also can be treated during the infusion. Following treatment patients will be tired for several hours and need to be accompanied home by a responsible adult. There are no long term side effects associated with Ketamine in the relatively low doses used to treat chronic pain. There is no chance of addiction to Ketamine.
Outcomes: Treatment protocols are individually planned depending on the nature of your pain and your response. In some cases a series of treatments will be recommended, often daily for a period of a week or more. The duration of pain relief following one or more ketamine infusions can not be predicted. The goal is to achieve lasting relief as measured in weeks or months following the last treatment. Most patients who enjoy prolonged pain relief will need to return on occasion for a booster infusion, or continue to take oral ketamine at home.
There is no guarantee that ketamine infusions will improve your chronic pain. Approximately 20% of patients will not experience relief. After the first two infusions together we will decide whether the continuation of ketamine therapy is right for you.
Because we cannot predict your response, the first two ketamine infusions will be at lower doses and of shorter duration. Starting with the third dose and thereafter, the duration of the infusions will average 3-4 hours for paients with CRPS / RSD reflex Sympathetic Dystrophy. The Ketamine dosage will be determined individually according to your pain response.
The Cost of Treatment:
Ketamine infusions is not covered by any insurance companies. Cost varies with problem being treated and length of IV therapy.
Ketamine: The Future of Depression Treatment? By Matt McMillen Reviewed by Michael W. Smith, MD Sept. 23, 2014 — Every year, 13 million to 14 million Americans have major depression. Of those who seek treatment, 30% to 40% will not get better or fully recover with standard antidepressants. That puts them at greater risk of alcohol and drug abuse, hospitalization, and suicide attempts. Now, though, a growing body of research shows there may be new hope: the anesthetic drug ketamine. Ketamine has a reputation as an illicit party drug due to its hallucinogenic effects. But in a handful of ketamine clinics around the country, people who weren’t helped by standard treatments are getting a series of infusions [typically 6] to ease their depression. The drug has also been used in emergency rooms for curbing suicidal thoughts, making it a potential lifesaver. “The benefits I’ve seen are pretty impressive, and the data are very strong,” says psychiatrist Kyle Lapidus, MD, PhD. He’s an assistant professor of psychiatry and neuroscience at Stony Brook University. Lapidus says there have been a large number of positive studies, though the number of participants in those studies has been small.
Ketamine acts quickly — often within hours or less — and health care professionals who give it to patients at therapeutic doses say it has mild and brief side effects in most people. But it hasn’t been thoroughly studied for long-term safety and effectiveness, and the FDA hasn’t approved it to treat depression. “The pace of research can be slow for people who are suffering,” Lapidus says. He says it’s not uncommon for doctors to go “off-label” (using a drug for a purpose other than its approved one) when treating patients. And in the case of ketamine, the research, including his own, has convinced him that it can help depressed patients. Lapidus runs a Manhattan clinic called US Ketamine. Soon, he will open a second clinic on Long Island. ‘Not a Miracle Drug’ Experts don’t know exactly how ketamine works, but they do know it works differently than commonly used antidepressants such as Prozac, Zoloft, and Effexor.
That may explain why people who aren’t helped by standard treatments respond to ketamine when other medications don’t help. That’s novel and exciting, says psychiatrist Alan Manevitz, MD. He specializes in treatment-resistant depression at Lenox Hill Hospital in New York. What’s equally noteworthy is ketamine’s ability to go to work right away, unlike most antidepressants, which take weeks, sometimes months, to provide relief. “Feeling better faster, getting the mood to improve faster — that’s why ketamine is very promising,” Manevitz says. He cautions, though, that no matter how successful ketamine proves to be, you can’t count on a single treatment to cure depression.
You need to address all aspects of a person’s disease, from the biological and the psychological to the social and environmental. “Ketamine is not a miracle drug at all,” Manevitz says. “It may momentarily take them away from that catastrophic place they’re in with depression, but you’re not addressing the rest of the patient. It’s a complex issue to treat psychiatric issues, and you have to treat the whole patient.” For people considering suicide, though, the drug’s rapid response could be life-saving. Recent studies have shown that a single dose of ketamine dramatically reduces suicidal thoughts. How long the drug’s effect lasts remains to be answered — a few days or weeks, it’s believed.
But that window of relief could prove critical. “We need suicide treatments so greatly in psychiatry,” says researcher Elizabeth Ballard, PhD. “Ketamine could be a bridge for someone who comes in who is suicidal. They are given ketamine, and for the 3 days or so that it’s effective, they can be hooked up with outpatient resources, with other medications, with psychotherapy.” Ballard, a researcher at the National Institute of Mental Health, published a study in August that shows ketamine reduces suicidal thoughts independent of its effect on depression or anxiety. That’s an important discovery, Ballard says, because not all suicides can be traced back to depression. Post-traumatic stress disorder, borderline personality disorder, and alcohol or other substance dependence, for examples, also account for some suicides. Further research is needed to explore the study’s findings.
Ketamine Clinics
While researchers continue to study ketamine, practitioners such as Lapidus have already begun to provide it to patients. The Ketamine Advocacy Network lists 17 providers and clinics around the country. Anesthesiologist Enrique Abreu, DO, runs the Portland Ketamine Clinic in Portland, OR. He works with a mental health specialist — Marilyn Sears, LCSW and clinic co-founder — and gives IV ketamine infusions. Most of his patients are self-referrals. “These people are suffering, and they find us online,” says Abreu, who estimates that he has treated 30 people since he opened his clinic 15 months ago. He says he has no mental health background, but he’s got 15 years’ experience using ketamine as an anesthetic. In fact, many clinic operators are anesthesiologists rather than mental health specialists. “It’s a weird gray area,” Abreu says. “Who’s going to help these people and do it safely?” Before Abreu treats someone, he consults with their psychiatrist or primary care doctor. Treatment then consists of six infusions over 12 days.
Each infusion lasts about 45 minutes. Side effects, which often include confusion, lucid daydreaming, and fuzzy vision, clear up quickly. Patients are watched closely and must have pre-arranged transport home. They’re barred from driving or using heavy machinery for 24 hours. Abreu says in his experience, the side effects “go away as soon as the infusion is over, and patients don’t have hallucinations.” Abreu says about three quarters of his patients aged 15 to 55 benefit from ketamine. Older patients have a lower response rate. The initial six infusions cost $3,800, the beneficial effects of which last anywhere from 3 to 5 weeks for some patients, and up to 12 weeks for others. Patients return as needed for single boosters, which cost $600. Because the FDA has not approved ketamine for this use, insurance doesn’t cover it. Lapidus says his clinic will mainly use a nasal spray form of ketamine, a method that he and his former colleagues at Mount Sinai’s Icahn School of Medicine found effective.
They published the results of their research in April. Manevitz, who has also used ketamine in his practice, says we don’t know anything yet about ketamine’s potential as a long-term treatment for depression. “The problem is maintaining the gain, prolonging the effect,” he says. Lapidus agrees: “How to maintain benefits: This is an area that needs a lot more research. Most of the studies published have involved only a single treatment.” A mind-altering drug called ketamine is changing the way some doctors treat depression. Encouraged by research showing that ketamine can relieve even the worst depression in a matter of hours, these doctors are giving the drug to some of their toughest patients.
And they’re doing this even though ketamine lacks approval from the Food and Drug Administration for treating depression. “It became clear to me that the future of psychiatry was going to include ketamine or derivatives of ketamine,” says David Feifel, a professor of psychiatry at the University of California, San Diego, who began administering the drug to patients in 2010. Ketamine was developed as an anesthetic and received FDA approval for this use in 1970. Decades later, it became popular as a psychedelic club drug. And in 2006, a team from the National Institute of Mental Health published a landmark study showing that a single intravenous dose of ketamine produced “robust and rapid antidepressant effects” within a couple of hours. Since then, thousands of depressed patients have received “off-label” treatment with ketamine.
One of those patients is Paul, 36, who lives in San Diego and is a patient of Dr. Feifel. We’re not using his last name to protect his medical privacy. Paul’s depression began with anxiety. “I was an extremely anxious child,” he says. “I would always make choices based on fear. My life was really directed by what was the least fearful thing that I could do.” As Paul grew up, his extreme anxiety led to major depression, which could leave him unable to get out of bed for days. “I lived in pain,” he says.
Paul managed to get through college and a stint in the Peace Corps. But most days were a struggle. And Paul has spent much of his adult life searching for a treatment that would give him some relief. He tried just about every drug used for depression, as well as cognitive behavioral therapy, acupuncture, and even electroconvulsive therapy, which induces a brief seizure. But nothing worked — at least not for very long. Paul says he was increasingly haunted by “this comforting thought of pressing a cold gun against my forehead where I felt the pain the most.” Then one day, while investigating depression on the Internet, Paul discovered the research on ketamine. “It was clear to me that this was real,” he says. Ordinarily, there would have been no legal way for Paul to get ketamine. He didn’t qualify for most research studies because of his suicidal thoughts.
And doctors usually won’t prescribe a mind-altering club drug to someone with a mental illness. But the studies of ketamine have produced results so dramatic that some doctors, including Feifel, are bypassing the usual protocols. By the time Feifel began hearing about ketamine, he had become frustrated with existing depression drugs. Too often, he says, they just weren’t helping his patients. David Feifel, a psychiatrist at the University of California, San Diego, has treated about 100 people with ketamine. A major study on antidepressant medication published in 2008 seemed to confirm his suspicions. It found that current antidepressants really aren’t much better than a placebo.
Many psychiatrists criticized that study. But not Feifel. “I was kind of like, I’m not surprised,” he says. “These really don’t seem like powerful tools.” Feifel remembers feeling “professionally embarrassed” that psychiatrists didn’t have something better to offer their depressed patients. Something like ketamine. He knew the drug had risks. It could be abused. It could produce hallucinations. And it didn’t have the FDA’s OK for treating depression. But he also knew that doctors had a lot of experience with ketamine. It’s been used for decades as an anesthetic that can rapidly stop pain without affecting vital functions like breathing. And ketamine’s safety record is so good that it’s often the painkiller of choice for children who arrive in the emergency room with a broken bone.
So in 2010, Feifel decided he wanted to offer low doses of the drug to some patients. The decision put him at odds with some prominent psychiatrists, including Tom Insel, director of the National Institute of Mental Health. “While the science is promising, ketamine is not ready for broad use in the clinic,” Insel wrote in his blog a few months ago. “There are a lot of pundits who remain skeptical or feel we need to research this ad infinitum before it’s ready, which doesn’t make sense to me,” Feifel says.
It’s hard to take the wait-and-see approach when you’re treating patients who are desperate for help, he adds. Paul was one of those desperate patients when he was referred to Feifel in March of 2014. The referral was from a local psychiatrist who had run out of ideas, Feifel says. And Paul jumped at the chance to try ketamine. “If there was even a 1 percent chance that this worked, it would have been worth it to me,” he says. “My life was hanging in the balance.” And for Paul, the benefits of ketamine became obvious soon after one of his early injections. “I remember I was in my bathroom and I literally fell to my knees crying because I had no anxiety, I had no depression,” he says. For the past year, Paul has been getting ketamine every four to six weeks. He feels an altered sense of reality for an hour or two after getting the drug. The effect on depression and anxiety, though, lasts more than a month. Ketamine doesn’t always work that well, Feifel says.
After treating more than 100 patients, he’s beginning to understand the drug’s limitations. One is that its ability to keep depression at bay can fade pretty quickly. Feifel recalls one patient whose depression would disappear like magic after a dose of ketamine. But “we could never get it to sustain beyond maybe a day,” he says. Shots – Health News Depression Treatments Inspired By Club Drug Move Ahead In Tests Also, ketamine treatment is expensive because patients need to be monitored so closely. Feifel charges about $500 for each injection and $1,000 for an intravenous infusion, which takes effect more quickly. Insurers don’t cover the cost because the treatment is still considered experimental. FROM KETAMINE PATIENT ADVOCACY NETWORK
Ketamine is “…the most important breakthrough in antidepressant treatment in decades” Thomas Insel, Director, National Institute of Mental Health What is ketamine? Can it relieve depression? Bipolar Disorder? PTSD? Anxiety? OCD? Migraines? About 70% of patients with treatment-resistant depression (including bipolar patients) experience rapid relief after a low-dose ketamine infusion. Similar success rates have been seen in returning combat veterans suffering from PTSD. These patients’ cases are the worst of the worst, lasting years or even decades, and which have not responded to any other treatments. Many have hovered on the verge of suicide for years, many have actually attempted suicide, and all have endured a very poor quality of life. Before ketamine therapy, there was virtually no way to substantially improve the condition of patients like these. The fact that ketamine works rapidly on 70% of them is astonishing, and its discovery has profoundly changed depression research, and our understanding of the very nature of depression.
It’s important to keep in mind, however, that the degree of relief can vary among patients. Some sufferers get only partial relief, some do not get relief until a second or third infusion, and some do not respond to ketamine at all. And some patients have additional medical conditions in addition to depression that can reduce its effectiveness. “The sense of wellbeing sneaked up on me. Instead of coming directly from the infusions like I expected, it came from doing all these new things that ketamine has freed me to do.” R.S., 30-year sufferer Ketamine patient since 2013 Is this real medical treatment, or just quackery? It’s real.
Ketamine treatment is an intravenous infusion procedure performed in a specially-equipped medical office by an MD, usually an anesthesiologist. It’s not hype. The National Institutes of Health has been studying ketamine’s affect on depression for more than ten years. There is serious scholarly research behind this treatment, which means controlled, double-blind, peer-reviewed studies at major institutions. Researchers at Yale pioneered this research nearly 20 years ago and published the first major study in 2000. Since then, dozens more ketamine studies have been conducted at Yale and other major institutions including NIH, The VA, Harvard, Johns Hopkins, Mt. Sinai Medical School, Oxford University, and many more around the world. What does relief feel like? The answer to that question is different for every patient.
The effects don’t always manifest themselves in the way you might expect. A lot of the ketamine buzz makes it seem like relief is instantaneous and total. But it’s important to keep realistic expectations based on facts, not hype. Yes, the relief is fast and it can be life-changing. But “fast” doesn’t always mean “instant”. Sometimes it takes several days to appear, and it might take multiple infusions. It might seem intermittent at first. Even if it takes several days, that is still warp-speed, comparatively. And the relief can be extremely subtle at first, building gradually instead of instantly overwhelming you. We’ll explain it by drawing on actual ketamine infusion patients.
This page is based on the experiences of real people, not hypothetical examples. Our ages range from 19 to 72. All of us all suffered extreme, treatment resistant depression (or bipolar or PTSD) lasting between 5 and 60 years. We include two university professors, a disabled US veteran, a PhD advisor to school districts, a small business owner, a retired programmer, a PhD neuroscientist, a corporate President/CEO, two college undergraduates, two single moms, and several people on Social Security disability due to their condition.
Nearly all of us experienced prolonged exposure to intense stress during childhood, or extreme trauma at some point in our lives. Our stories include combinations of physical abuse, emotional abuse, sexual abuse, neglect, the murder of a loved one, having an alcoholic or addicted parent, being in violent military combat, having an imprisoned parent, and much more.
All of us tried the usual meds and therapies for years. We were mostly unable to function normally, causing many of us to lose nearly everything we held dear: marriages, family relationship, jobs, homes, friendships, a sense of belonging, etc. About half of us had attempted suicide resulting in hospitalization; and in some cases multiple attempts. Each of us was acutely miserable immediately prior to our first infusion. Our symptoms were typical for patients like us: anhedonia, anxiety, dysphoria, irritability, insomnia, fatigue, social phobia, cognitive impairment, etc. Some of us responded immediately, and felt relief within hours. Others didn’t feel anything until a few days later, or until after the second or third infusion. In one case, it took four infusions, but then the relief was solid. Some described their relief as total, others partial. Keep in mind that to someone who is in acute agony, even partial relief can be life-changing. Also keep in mind that some patients do not respond to ketamine, and here we are only talking about those who do.
We ask many successful patients “If you could travel back in time to before your infusion, how would you explain the relief in terms your depressed self could understand?” Most say it’s impossible. They say the explanation would be incomprehensible to their depressed self, and the only way to understand it is to experience it.
We’ll try to explain it anyway… Relief of Symptoms You might not think of your depression/bipolar/PSTD as a collection of symptoms. To you it might simply feel like the way you interact with the universe, like it’s part of your very identity.
But how many of these typical symptoms apply to you? •anhedonia •anxiety •fatigue •irritability •feelings of sadness, emptiness •insomnia, or excessive sleep •difficulty concentrating and making decisions •feelings of guilt or worthlessness •social avoidance •thoughts of suicide
If those symptoms were relieved, would you still be depressed? In the simplest terms, ketamine relieves symptoms. It doesn’t add something new to your personality that causes instant happiness. It just takes away some horrible symptoms. You think you’d notice immediately when these symptoms vanish. Not always. The sensation can be incredibly subtle. There is no jolt of giddiness that instantly courses through your system. The sensation is deeper than that, and gentler. When symptoms are relieved, patients can quickly gain new abilities that were previously impossible.
Like casually picking up the phone to call a friend. Or suddenly breaking out of persistent negative thought loops or behaviors. Or simply being able to get out of bed and stay productive throughout the day.
Let’s go a little deeper… Mood vs. Function When we talk about ketamine relief, keep in mind the difference between your mood versus your function. It’s important. Most of us think of depression/bipolar/PTSD as something that makes us feel horrible, where our mood is bleak. But the impact is in how it prevents us from functioning normally.
It impairs us so we can just barely socialize, work, take care of ourselves, maintain relationships, keep our lives organized or our homes clean, etc. – and sometimes not at all. Our lack of function makes our mood even worse, which creates a vicious cycle. Most patients go into ketamine therapy focused on their mood. Understandably, they are desperate to feel better. They hope to be overwhelmed with an obvious, electrifying sense of relief.
They’ve heard that ketamine can create a miraculous feel-good sensation. One prospective patient said “I imagine the doctor pouring a quart of happiness into my veins, and I’ll be able to feel it coursing through my body afterward.” It doesn’t work that way. Most successful patients do not get an instant, obvious, smack-you-in-the-face sense of total recovery. Relief usually comes without the jolt. Sometimes it takes multiple infusions and several days (which is still incredibly fast, after years of suffering). Instead of an instant smack in the face, relief usually reveals itself in a different way – more subtle, yet still profound.
Here’s a typical expectation of a first-time patient: After the infusion I will instantly have an acute sense of relief. This will lift my spirits and make me feel happy. Then my new mood will make me function better and I’ll become productive. Here’s what the same patient might say after successful treatment, looking back after some time has passed: After the infusion I had trouble detecting instant changes. I didn’t get an obvious thunderbolt of happiness, so I thought the treatment failed. Then I started noticing I was functioning better, doing things that used to be terrifying or impossible, but surprisingly it didn’t seem like a big deal. The more I exercised these new abilities, the more I realized this was a huge improvement. I started to feel a deep satisfaction that I was functioning well, and that something at my core had truly improved. This made me feel healthy and happy. It’s very important to understand that function often improves before mood.
We’ve seen many first-time patients turn all their thoughts inward and search intensely for obvious feelings of happiness. If they don’t find it quickly, they can become despondent because they pinned so much hope on ketamine therapy, and now they think it failed. By focusing solely on their mood, they often don’t notice improvements in their function. In fact, friends and family often notice the function improvements before the patient does – this is very common. Once the patient finally recognizes they are functioning better, even just a little bit at first, it’s very likely to trigger strong improvements in mood – and they’ll get the sense of happiness they expected in the first place. But what do we mean by “improved function?” Here are some examples given by actual ketamine patients:
- Being able to genuinely feel positive emotions, without faking it
- Being able to socialize with friends and family, and truly enjoy it
- Stresses and obstacles roll off your back instead of reducing you to the fetal position
- Finding it easy to sleep right, shower every day, and take care of yourself
- Having enough physical energy to get through the day without constant exhaustion
- Finally finishing projects that have dragged on for months or years, like home repairs, housekeeping, organizing finances, etc.
- Interacting comfortably in big groups, or with strangers, without social anxiety
- Criticism and unkind words become things you can simply shake off, instead of causing deep wounds that won’t heal
- No more energy spent trying to block out certain memories or traumas; they’re just not terrifying anymore
- No longer intimidated by authority figures, bosses, etc.
- Suddenly “getting” what your therapist has been saying for years It seems like any of those improvements would hit you like a ton of bricks, and you’d recognize it immediately.
But fellow patients will tell you these changes can be incredibly subtle at first. They can sneak up on you. It’s counter-intuitive, but it’s just simply a fact of ketamine therapy. A couple of actual patient quotes summarize it nicely: Patient R.S., male, suffered 30 years: I can’t believe the huge difference these tiny gains have made in my life. I thought ketamine would give me an instant sense of wellbeing that I could feel in my gut, and then I would use it like a weapon to conquer the world and do the things I want. But it actually worked the other way around. Ketamine gave me the ability to do a bunch of small routine things that I could never do before, and together they’ve made my entire life easier. The sense of wellbeing sneaked up on me.
Instead of coming directly from the infusions like I expected, it came from doing all these new things that ketamine has freed me to do. Patient S.P., female, suffered 20 years: I thought I’d be blasted with relief. Like from a fire hose. I squinted my eyes and tensed up waiting for the blast. The longer I waited the more tense I got. It distracted me from the pool of relief that formed silently under my feet over the course of three infusions. I didn’t notice it until I was completely soaked from the bottom up. Frankly I was disappointed because I imagined the blast would be so awesome. But once I realized I was drenched in relief and was actually functioning and living life again, the blast seemed pointless. We know how hard it is to be patient after your first treatment – we’ve been there.
But many patients before you have been through this, and you can benefit from their experience. Relief doesn’t always come as instant happiness. For many patients it comes as an improvement in function over several days, which in turn lifts your mood. Please take this to heart, and keep your expectations in check during your initial treatment phase. Lasting Benefits, Even After Relapse When a patient experiences relief like we’ve described, they can often make huge sudden leaps forward in their emotional healing. Some patients have spent their entire lives suppressing traumatic memories, or nurturing hatred towards an abuser. They may be wracked with guilt over lost relationships, or may be despondent from losing precious years of their lives. When relief lifts a patient’s function and mood, they can have a sudden profound shift in the way they view life itself, and how they fit into the universe.
A sudden positive shift in how you see things It’s hard to truly understand if you haven’t been through it. There’s a lot of variation among patients, of course, but there is a common theme. In their pre-ketamine suffering, many feel like a walking defect, an uninvited and unwanted guest wherever they go. But in their relief, this can be replaced by a sense of belonging, like they are a valued member of the human race, and that they are wanted. This can set the stage for sudden shifts in the way a patient views the world and his/her place in it. That might include social phobia giving way to a desire to interact with new people, or letting go of toxic hatred toward an abuser, or coming to terms with a horrible trauma so it stops being a constant source of terror.
It doesn’t mean they suddenly become happy about everything in their past. But it means they can suddenly understand and accept it in a way that was impossible before. They can make peace with traumas, failures, regrets, etc., that have hijacked their thoughts for years. In this state, many patients say they suddenly “get” what their therapists have been saying for years. If you have a competent therapist, this is the perfect time to tackle your emotional issues. By building on symptomatic relief, improved function, and newfound resilience, effective counseling at this stage can help you make deep, lasting gains. Some ketamine responders have told us they made more emotional progress in a few months of post-infusion counseling than all the years prior.
Patients who have these massive shifts often find they are permanent. Even if their individual symptoms return, many of these patients have lasting benefit from these shifts. Their improved, healthier thought patterns make them more resilient, and help them contend with the symptoms better than before. And some long-term infusion patients say that repeated cycles of relief/relapse help this resilience to increase over time. This is one of the best possible outcomes of successful ketamine therapy. It doesn’t happen for every patient. Many patients get tremendous relief even without this effect. If it happens for you, great – but it’s not a requirement for success.
A Metaphor for Ketamine Relief People with depression/bipolar/PTSD often feel trapped. Imagine you’re in a hedge maze where you can’t see over the hedges. All you can see are the leafy green walls surrounding you. How will you get out? The only thing you can do is wander aimlessly until you encounter a juncture. But then which path should you take? You still can’t see anything except what’s right in front of your nose, so you can’t make a plan that considers the big picture. All you can do is guess at the right direction.
Your odds of escaping are slim. You’ll be stuck in a never-ending loop: wander aimlessly, stumble across a juncture, pick a random direction, wander some more. But other people in the maze are tall enough to see over the hedges. They can see where the exit lies. They can see exactly how to get to the next juncture, and which way to turn when they get there. To them, it’s easy. You’ll be exhausted from wandering and backtracking. You’ll be embarrassed each time someone breezes past you. Trapped in the maze long enough, you’ll eventually forget you ever knew anything besides futility, hopelessness, shame.
When ketamine relieves depression it’s like suddenly being able to see over the hedges. Now you can see the exit. Now you can function like everyone else. It doesn’t matter how long you’ve been trapped or how hopeless you’ve become – once you get a birds eye view, charting your course out is straightforward. In this metaphor, your “symptom” was not being able to see over the hedges. Once that was relieved, you were able to function normally and get yourself out. No superpowers were needed, like being able to fly over the maze or blast your way through. Removing your symptom allowed you to do it in a matter-of-fact way, under your own power. Successful ketamine therapy is like that.
The “Crash”
Some patients feel initial relief, but then have the sensation that it disappears suddenly after a day or two. This can be very upsetting. Relief makes you start to feel hopeful again, maybe for the first time in years, so imagine your sense of loss if it vanishes quickly. We have a suspicion as to why this occurs. We’re not doctors or researchers, and our suspicion isn’t science. It’s just an informed hunch based on our experiences as patients who collectively have been through dozens of infusions.
First, it’s important to know that most patients who experience The Crash ultimately declare their treatment a success. At some point after The Crash, they feel relief again – maybe in a slightly different form. Here’s our hunch… For some patients, the symptomatic relief produces definite physical sensations. It’s not subtle. They feel an acute awareness that their anxiety is missing, for example. Or that their dysphoria is reduced. Sounds great, right? But for a subset of these patients, after a day or so, the acute symptomatic sensation fades. We suspect this fading is The Crash. But even after The Crash, most of these patients go through the exact same progression described above. First they’ll gradually notice that they’re functioning better, which in turn will lift their mood, and so on. We simply want you to be aware this phenomenon can occur. If it happens to you, keep in mind that many other patients have been through The Crash yet still ultimately achieved solid relief.
Conclusion: Consider relief to be a spectrum of results. The very best outcomes might include a rapid, obvious reduction of symptoms; increased function and productivity; significant improvement in mood; and a massive positive shift in the patient’s fundamental thinking that persists even after relapse. Not everyone will get this best-possible case. But to patients who’ve suffered years in acute agony, even partial relief can be miraculous and life-changing. Most first-time ketamine patients are desperately craving relief. They can’t help but pin all their hopes on this new option. It’s completely understandable for someone who’s suffered for years, maybe decades, where no treatment has ever helped. When the stakes are so high, expectations can run wild.
We want to be blasted with relief, instantly. We might fantasize that it will arrive in dramatic fashion, with an incredible electric sensation, and gasps from spectators. Relief rarely comes in that packaging. It’s usually much more subtle – but just as gratifying. Many patients get incredible, life-changing relief without pyrotechnics. Honestly, it’s hard to understand until you’ve been through it yourself. We’ve done our best to explain it, but if you want to make sure your expectations are realistic, ask a question in the discussion forums or talk to your ketamine provider. “I wish I could have tapped the wisdom of other patients before my first treatment but there just weren’t very many of us then. I could have prepared better if I knew then what I know now.” Dennis Hartman Founder/CEO, Ketamine Advocacy Network
Getting The Most Out Of Treatment If you’re going to spend serious money and pin your hopes on being a ketamine responder, you should do everything in your power to get the most out of the treatment. Here we’ll share some practical experience from a variety of patients. Between us, we’ve had many dozens of infusions, and have picked up some do’s and don’ts along the way. Some of us did not feel our treatment was successful at first, but later recognized solid improvement. There are things you can do before, during, and after treatment to maximize your chances of a good outcome. Keep in mind that some patients do not respond to ketamine, and here we are only talking about those who do.
Rest Up Try to be well-rested before the infusion. If you have a morning appointment and are worried about being able sleep the night before, ask your ketamine provider if it’s ok to take a sleep aid. Some patients feel their infusions are less effective when they are sleep-deprived.
Relax Empty your bladder The infusion only puts a few ounces of fluid into your body. But many patients feel like their bladder is full as soon as the infusion is over. Make sure it’s completely empty before the infusion starts, to buy yourself time at the end of the infusion before you have to make your way to the bathroom. We realize this is easier said than done for some patients, but try to be in a relaxed state before the infusion starts. Patients who are very tense when the treatment starts are more likely to have brief moments of unpleasantness during the infusion. If caffeine makes you jumpy, maybe skip your daily cappuccino or wait until after your appointment. Obviously, you may be pinning a lot of hopes on the treatment and that can make you anxious. Arming yourself with knowledge about the treatment and setting realistic expectations can help you relax when you get there. (Do not take a benzodiazepines to relax before your appointment! See below.)
Ask If Your Current Meds Will Interfere Make sure your ketamine provider is aware of every drug you are currently taking, whether it’s a psychotropic med, heart medication, cough syrup, an illegal substance, etc. Some substances can interact with ketamine or interfere with its action in the brain. For example, high doses of benzodiazepines seem to reduce ketamine’s antidepressant effect. If you are taking a daily high dose of benzodiazepines, your doctor might recommend reducing it before your treatment (he/she probably won’t ask you to stop taking it completely). Other meds that can impact ketamine’s efficacy include lamotrigine [Lamictal], memantine, and any drug that affects NMDA receptors. Don’t hold anything back from the doctor. There’s no point investing your money and hopes unless you’ve disclosed everything and your doctor is satisfied nothing will interfere with the ketamine.
Bipolar Manic State
There is a lot of research showing ketamine is effective for bipolar patients. But some researchers say bipolar patients get good results only when their infusion happens during a depressed state, not manic. If you are bipolar and are in a manic state on the day of your appointment, make sure the doctor is aware. Together you may decide it’s better to postpone until you cycle back to depressed.
Tell Your Loved Ones to Hold Their Questions
Easy to ask, hard to answer. Ask your friends and family not to bombard you with questions after the treatment. They will naturally want to ask “Did it work?” or “Do you feel better?” But the effects can be extremely subtle at first and many patients have trouble putting the experience into words. You may need time to process it. Even those who can sense an immediate change often find it impossible to articulate at first. When people ask those questions it can make you feel pressured not to disappoint them. To them, these seem like easy questions, but to you the answers may be complicated in ways you can’t explain. Let them know ahead of time that you’ll talk about it when you’re ready, which might take a few days. Don’t Stress Out Waiting for a “Blast” of Relief – Remember Function Often Improves Before Mood Don’t forget that successful patients often begin functioning better before they feel better.
We’re serious: do NOT forget this fact while you wait for relief to reveal itself. You might be inclined to find an isolated place, close your eyes, block out all noise, and concentrate hard to measure your mood, searching for any tiny changes. It’s perfectly understandable why, but doing that won’t actually help you. Instead, try to go about your daily routine. You may gradually realize that it’s easier than before. Even if your daily routine was nothing but lying in bed wishing you could get up, you may start noticing small things becoming easier, like putting on clothes, brushing your teeth, etc. These improvements can snowball in ways you don’t expect. Many patients look back later and recognize small improvements like these as the first signs of relief, even if they didn’t seem momentous at first.
Put Your Improved Function to Use – Right Now! If you respond to ketamine, you will be able to function better than before. Put that ability to use! Don’t wait, even for a minute. If you’re able to socialize, go do it right now, instead of just patting yourself on the back for feeling able. If you’re able to clean your house or organize your finances, do it right now, instead of feeling satisfied that you could do it. The more you exercise your improved function, the more your mood will lift. Imagine you had a muscle-wasting disease instead of depression, but there’s a treatment that can quickly repair the damage. If you don’t put those newly-repaired muscles to use, your treatment was wasted.
But if you lift weights and focus on building new muscle mass, you’ll be much more able to deal with the condition if it returns, literally from a position of strength. Successful ketamine therapy gives you the ability to build new “muscle” in the form of better function, improved habits, etc. – and the improved mood that comes with those things. This combination can give you an entirely new power: resilience. If your depressive symptoms return, your new strength and resilience can help you withstand those symptoms better than ever before. Most responders do not sink all the way back to their old baseline.
In our experience, the likelihood of permanent baseline improvement is directly related to how much you exercise your improved function while the relief holds, regardless of whether it lasts one week or six months. Build on Your Relief to Make Lasting Emotional Gains When a patient experiences relief like we’ve described, they can often make huge sudden leaps forward in their emotional healing. Many patients say they suddenly “get” what their therapists have been saying for years. Take advantage of this state and find a competent therapist who can help solidify your benefits into lasting emotional gains. Many patients find these improvements persist even if their symptoms return, giving them a resilience they never had before.
Concerns Regarding Ketamine
- Consequences of long-term use have not been studied yet. That statement is true. There are no studies on long-term repeated ketamine infusions for depression. And there probably never will be, for the reasons explained in the Big Pharma section. There is simply no way to turn ketamine into a big moneymaker, so no one is going to fund that research. Instead of researching long-term ketamine use, or trying to find the most effective dosage and infusion schedules, much of the research is heading in a different direction. The search is on for other drugs that are similar to ketamine, but different enough to be patented. In other words, ketamine-like drugs that could become blockbuster moneymakers. If such a drug is found and obtains FDA approval, it will quickly become one of the top 5 or 10 bestselling drugs in the world, even if it proves less effective than ketamine. Some of the research remains focused on the underlying ketamine mechanisms of action, but enough effort has shifted towards profit to dilute the resources available for fundamental science. Bottom line: we’re not aware of a single study, current or planned, that looks at potential consequences long-term ketamine therapy – there is simply no appetite for this research. Even though there are no formal studies on long-term infusions, there is actually quite a lot of good clinical data available. For 20 years, ketamine infusion has been the most effective treatment available for Chronic Regional Pain Syndrome (CRPS), also known as Reflex Sympathetic Dystrophy (RSD), an extremely painful neuropathic condition. The ketamine dose in a typical CRPS infusion is between 2x and 10x that of a depression infusion. And they are much more frequent, sometimes with multiple infusions per week, where a depression patient may get 1-2 infusions every few months. Yet after 20 years of routine CRPS use there is no clinical evidence of negative side-effects from repeated infusions. Can’t wait for long-term study of life preservers. Let’s talk about what we do know. Ketamine has a 50-year track record as a safe anesthetic, and a 20-year history as a safe long-term CRPS treatment. It’s proven to rapidly relieve depression/bipolar/PTSD symptoms in about 70% of treatment-resistant patients for whom no other treatment works. Most importantly, we know the awful consequences when patients like us can’t get relief. Finally, substantial research has shown that living with severe depression causes measurable physical injury to the brain. Every day that passes without relief means additional harm to the brain. With ketamine treatment, there’s a chance of relief. Without it, there’s guaranteed continued suffering. Patients must be entitled to weigh the risks for themselves.
- The relief is not permanent, and depressive symptoms will return for most patients. This statement is true. But so what? Do psychiatrists discourage patients from taking SSRIs because a single dose can’t permanently extinguish their symptoms? Taking a single dose of insulin doesn’t cure diabetes, but is that a reason not to take it? No one is hawking ketamine as a cure. It’s a treatment. An intervention. That’s why it’s called “therapy,” not a “permanent fix.” Yes, the patient will usually relapse, at least partially. But most find additional treatments will restore the relief. Ketamine can have lasting benefit even after relapse occurs. When ketamine relieves their symptoms, many patients find they are suddenly able to achieve rapid, profound emotional healing, and break out of negative behaviors and thought loops that were previously inescapable. When the symptoms begin to return, the emotional healing can persist. It can make the patient more resilient, and better able to withstand the pain caused by the symptoms.
- Dissociation is an unacceptable side-effect. Is puking violently for days an acceptable side-effect of lifesaving chemotherapy? What about losing your hair for a year? Who decides? Is 40 minutes of mild dissociation an acceptable side-effect of lifesaving ketamine therapy? Again, who decides? Many medical treatments have truly awful side-effects, yet they are universally embraced because the benefits dwarf the side-effects. Chemotherapy and radiation treatment are two examples. Ketamine therapy is like that too, where the magnitude of the dissociative side-effect is trivial compared to the life-changing relief it provides many patients. Unlike chemo or radiation, this side-effect is brief, disappearing completely once the infusion ends. Moreover, ketamine patients usually experience dissociation as a pleasant side-effect, not negative. To declare it an “unacceptable” or “negative” side-effect is to pass a moral judgment, and that is outside the jurisdiction of researchers. Doctors, pharmaceutical companies, and other parties also have no business telling patients which side-effects are acceptable in exchange for relief. Patients must be entitled to decide for themselves which side-effects are worth the potential payoff. One lifelong sufferer told us “If I could relieve my depression by gnawing off my own limbs, I would do it in a heartbeat.” There’s simply no way to argue that this patient’s misery is preferable to a brief dissociation. “We give chemotherapy for cancer and there are side effects with chemotherapy, but we give it anyway, because people need it to get better from cancer. Ketamine does not have the side effects chemotherapy does, yet we’re using it for a disease that has a defined mortality; there is a suicide rate associated with severe depression.” Dennis Charney Co-author of the original Yale study and Dean of Icahn School of Medicine at Mt. Sinai
- Infusions are too much of a hassle. Patients need something that is easier to administer. Of course it would be preferable to have something simple like a pill. But until the research produces something easier to administer that is just as effective as ketamine, what’s the alternative? Remember we’re talking about patients who respond to no other treatment. They’ve already exhausted the usual options, and they deserve a lifeline. The right to decide whether infusion is worth the trouble lies solely with us, the patients. As soon as something better comes along, we’ll be the first in line. Until then, the hassle of an infusion is a very small price to pay when it can literally save lives and restore happiness.
- Reckless clinical use of ketamine could cause a PR backlash. Researchers fear that a ketamine clinic might use ketamine recklessly in a way that causes a patient harm. The media could seize the story and create a powerful negative buzz. Imagine such a story in the hands of a news org more interested in click-based revenue than accuracy or completeness. They won’t bother to convey the complexities of the issue or balance the story with examples of patients whose lives were saved by ketamine. They will hype the fact that ketamine is abused illegally, and ignore the fact that medical use dwarfs street abuse by 10000-to-1. They’ll call it a party drug and horse tranquilizer. A single story could be hyped in a way that taints the entire ketamine field. It could make it harder for researchers to conduct their work, and harder for conscientious ketamine clinics to treat patients. We share this concern. In fact, there are some clinics that we feel use inappropriate protocols or have poor standards of care (they do not appear in our directory) and we are deeply concerned they will cause the sensationalistic story we dread. But patients like us are dying in appalling numbers, leaving behind shattered families and whole new crops of sufferers in the wakes of their suicides. Children who lose loved ones commit suicide are at very high risk of becoming lifelong sufferers themselves. We can’t afford to wait for the public policy issues to be debated to everyone’s satisfaction. It’s immoral to deny us a last-ditch lifeline that has been conclusively proven effective. This concern is legitimate, but it must be addressed in a way that doesn’t rob sufferers of access to the treatment.
From Physician Weekly
Ketamine Works in OCD, Stubborn Depression
by SkepticalScalpel | May 21, 2013 | Articles, Conference Coverage Releases, Depression, Psychiatry, 1 comment SAN FRANCISCO — The anesthetic agent ketamine continues to show tantalizing promise in psychiatric disorders, with results from new studies in intractable depression and obsessive-compulsive disorder (OCD).
In a 72-patient randomized trial involving patients with major depression who had not responded to standard therapies, mean scores on the Montgomery-Asberg Depression Rating Scale (MADRS) fell by half 1 day after an intravenous infusion with ketamine, significantly more than in an “active placebo” group receiving the benzodiazepine agent midazolam.
The ketamine group continued to show significantly greater improvement for the next 2 days relative to the controls, according to James W. Murrough, MD, of Mount Sinai School of Medicine in New York City.
A second trial in 15 patients diagnosed with obsessive-compulsive disorder, conducted at Columbia University in New York City, found that the drug was significantly superior to placebo (saline, in this case) in reducing OCD symptoms according to the Yale-Brown rating scale and patient self-assessments.
Both studies were reported here at the American Psychiatric Association annual meeting.
Ketamine for Depression
All current antidepressant drugs — tricyclics, monoamine oxidase inhibitors, and inhibitors of serotonin and/or norepinephrine reuptake — require a minimum of several weeks before clinical benefit is apparent. Suicidal ideation is a recognized risk during this period. Consequently, an antidepressant with a more immediate onset of action would be eagerly welcomed.
Ketamine drew attention as a possible candidate in 2006 when a small placebo-controlled trial conducted by the National Institute of Mental Health (NIMH) researchers found that ketamine induced dramatic improvement in depression scores within 2 hours of IV infusion, and which lasted for a week.
Subsequently, another placebo-controlled study by the NIMH group found nearly instant relief with ketamine in bipolar patients with severe depression
The depression study by Murrough and colleagues was an attempt to improve on the NIMH studies by using a psychoactive drug as the control instead of saline. Murrough said that blinding in the earlier studies might have failed because of ketamine’s distinctive psychotropic effects.
In fact, ketamine is available on the street because it can produce a “high” marked by out-of-body dissociative sensations along with euphoria and other perceptual effects. These are among the reasons that ketamine has not already gained traction as an antidepressant.
Murrough said he and his colleagues selected midazolam as the control in their study because it could also be perceived by participants as an active drug, yet without either depressant or antidepressant effects. Its mechanism of action is also different from that of ketamine, an antagonist of so-called NMDA glutamate receptors.
Participants in the study, recruited and treated at two different clinical sites, were assigned in a 2:1 ratio to ketamine at 0.5 mg/kg or midazolam at 0.045 mg/kg by IV infusion.
Patients had long histories of major depressive disorder, with mean duration of more than 20 years. About one-third had attempted suicide at least once and half had a history of psychiatric hospitalizations. Participants had failed a mean of five previous antidepressant treatments.
Mean MADRS scores at baseline were 32.6 in the ketamine group and 31.1 among controls. The next day after infusion, the mean scores declined to 16.1 with ketamine versus 22.3 for controls.
After adjusting for baseline differences between groups and the two clinical sites, the difference in change from baseline in MADRS scores between arms was statistically significant atP=0.0014.
Based on Clinical Global Impression scores for improvement and severity, 64% of the ketamine group and 28% of those receiving midazolam were judged to be responders at the 1-day evaluation (P=0.006).
The advantage of ketamine over midazolam was maintained through day three post infusion. At day seven, 46% of the ketamine group was still considered to be responders versus 18% of controls, but the difference was no longer significant.
MADRS scores also rebounded slightly by day seven, enough to render the advantage over midazolam insignificant.
Ketamine for OCD
Carolyn Rodriguez, MD, PhD, of Columbia told MedPage Today that dysregulation of excitatory glutamate receptors appears to play a role in OCD, prompting their look at ketamine as a potential treatment. The drug had already shown promise against OCD in a case study and a small open-label trial.
The Columbia group randomized 15 patients to a single infusion of ketamine or conventional placebo on a crossover basis, with at least 1 week (mean 2.1 weeks) between treatments.
Patients had mean Yale-Brown scores at baseline of 27 (SD 3), indicating moderate to severe illness. They had tried an average of three previous treatments without durable success.
As in the depression studies, the effect was immediate. Using a visual analog scale, patients reported dramatic decreases in their obsessive-compulsive urges midway through the 40-minute infusion. The self-assessed effect remained greater for the drug versus placebo through a full week. Because the effect appeared to last beyond 1 week, results from second, post-crossover infusions were not used in the analyses. Rodriguez told MedPage Today that the durability of ketamine’s effects, both in OCD as well as in depression, remains a mystery. The drug has a very short half-life in circulation — measured in minutes — and yet its clinical effects last for a week or more. Ketamine’s apparent efficacy in OCD also underscores possible similarities to depression in the underlying biology. Currently, the first-line drug treatment for OCD is antidepressants, Rodriguez noted.
Next Steps
For next steps, she said, she was most interested “in elucidating mechanisms — why some people respond to [ketamine] but not all, and what is the mechanism of the rapid effect and what is the mechanism of action of the sustained effect.”
She added that another important follow-up will be to determine whether there are other ways to modulate the NMDA receptor to achieve the same benefits without causing the dissociate symptoms and other unwanted effects.
Murrough said that, in fact, it’s still not entirely clear that ketamine does work through NMDA receptors. Although that appears to be its principal target as an anesthetic, “ketamine is a dirty drug,” he said, with effects on other neurotransmitter systems besides glutamate. Carlos Zarate, MD, the NIMH researcher who led the earlier studies, told MedPage Today that the ketamine studies were one of the few bright spots on the pharmacological front in all of psychiatry. The dearth of new drug classes for major disorders has been a common lament in recent years.
Although most ketamine studies to date have remained small pilot trials, Zarate said he was not discouraged at the pace of progress. He said NMDA is a complex target that has proven to be difficult to modulate in exactly the desired way. Drug companies have been trying for decades to develop NMDA-active drugs, and have renewed those efforts as the basis of the ketamine studies.
Although the earlier efforts mostly didn’t pay off, researchers both in and out of industry have many more tools at their disposal, Zarate said. Several promising compounds have been reported by drug firms.
In the meantime, ketamine itself may be clinically acceptable for patients with severe depression, as the benefits could outweigh the adverse effects. He noted that it has been effective in patients unresponsive to electroconvulsive therapy, currently the treatment of last resort for severe depression. Zarate said the dissociative symptoms are disconcerting during the first treatment, but become less so when patients know what to expect. Another researcher presenting at the APA meeting, Delisa Guadarrama, MD, of the University of Texas Health Sciences Center in San Antonio, said the dosing regimen is another area to be investigated further. She reported on a case of severe postpartum depression, in which she and colleagues treated the patient with 2 mg/kg of ketamine — four times the dosage used in most previous studies. Guadarrama said that the woman was being treated in the center’s pain clinic, where the higher dose was customary. Her patient, as well as patients with other types of depression also treated with 2 mg/kg, showed symptom relief lasting for 3 weeks or longer, in contrast to the 1-week duration of effect seen with the 0.5-mg/kg doses. Vital signs did not indicate any greater degree of adverse effects than in reports with the lower dose, she said. Whether the dissociative symptoms were more severe would be more difficult to assess, since no quantitative tools for measuring these symptoms are available. KETAMINE IMPROVES DEPRESSION in BIPOLAR Patients within minutes Antidepressants are commonly prescribed to treat or prevent the depressive episodes, but they are not universally effective. Many patients still continue to experience periods of depression even while being treated, and many patients must try several different types of antidepressants before finding one that works for them. In addition, it may take several weeks of treatment before a patient begins to feel relief from the drug’s effects. For these reasons, better treatments for depression are desperately needed. A new study in Biological Psychiatry this week confirms that scientists may have found one in a drug called ketamine. A group of researchers at the National Institute of Mental Health, led by Dr. Carlos Zarate, previously found that a single dose of ketamine produced rapid antidepressant effects in depressed patients with bipolar disorder. They have now replicated that finding in an independent group of depressed patients, also with bipolar disorder. Replication is an important component of the scientific method, as it helps ensure that the initial finding wasn’t accidental and can be repeated. In this new study, they administered a single dose of ketamine and a single dose of placebo to a group of patients on two different days, two weeks apart. The patients were then carefully monitored and repeatedly completed ratings to ‘score’ their depressive symptoms and suicidal thoughts. When the patients received ketamine, their depression symptoms significantly improved within 40 minutes, and remained improved over 3 days. Overall, 79% of the patients improved with ketamine, but 0% reported improvement when they received placebo. Importantly, and for the first time in a group of patients with bipolar depression, they also found that ketamine significantly reduced suicidal thoughts. These anti-suicidal effects also occurred within one hour. Considering that bipolar disorder is one of the most lethal of all psychiatric disorders, these study findings could have a major impact on public health. “Our finding that a single infusion of ketamine produces rapid antidepressant and anti-suicidal effects within one hour and that is fairly sustained is truly exciting,” Dr. Zarate commented. “We think that these findings are of true importance given that we only have a few treatments approved for acute bipolar depression, and none of them have this rapid onset of action; they usually take weeks or longer to have comparable antidepressant effects as ketamine does.” Ketamine is an N-methyl-D-aspartate (NMDA) receptor antagonist, which means that it works by blocking the actions of NMDA. Dr. Zarate added, “Importantly, confirmation that blocking the NMDA receptor complex is involved in generating rapid antidepressant and anti-suicidal effects offers an avenue for developing the next generation of treatments for depression that are radically different than existing ones.” Story Source: The above post is reprinted from materials provided by Elsevier. Note: Materials may be edited for content and length. Journal Reference: Carlos A. Zarate, Nancy E. Brutsche, Lobna Ibrahim, Jose Franco-Chaves, Nancy Diazgranados, Anibal Cravchik, Jessica Selter, Craig A. Marquardt, Victoria Liberty, David A. Luckenbaugh. Replication of Ketamine’s Antidepressant Efficacy in Bipolar Depression: A Randomized Controlled Add-On Trial. Biological Psychiatry, 2012; 71 (11): 939 DOI: 10.1016/j.biopsych.2011.12.010
